Transfer Drg Definition

Medicares DRG system is called the Medicare severity diagnosis-related group or MS-DRG which is used to determine hospital payments under the inpatient prospective payment system IPPS.
Transfer drg definition. Incorrectly coded claims can result in lost Transfer DRG payments as high as 70k per account. 011 Tracheostomy for face mouth and neck diagnoses or laryngectomy with mcc. Medicaid Services CMS did some studies that indicated many patients admitted to an acute hospital were transferred shortly after admission to post-acute care creating an overpayment to the acute care hospital or as some authors have described it a.
The relative volume and types of diagnostic therapeutic and bed services used in the management of a particular illness. Certain DRGs known as Transfer DRGs are paid under the Medicare Post Acute Transfer rules which reduce payments for hospitals that transfer patients to other providers to continue treatment. 5282014 Because they felt Medicare was paying twice for the treatment of certain patients CMS officials adopted the Post-Acute Transfer PACT rule.
The issue of a check constitutes an authority for collection by debit transfer. In some cases only high dollar impact claims and obvious underpayments are examined during a primary review. A DRG is a grouping of similar clinical conditions diagnoses and the service procedures furnished during the inpatient hospital stay.
013 Tracheostomy for face mouth and neck diagnoses or laryngectomy. Its the system used to classify various diagnoses for inpatient hospital stays into groups and subgroups so that Medicare can accurately pay the hospital bill. Rehab hospitals skilled nursing facilities long-term care hospitals or home health care.
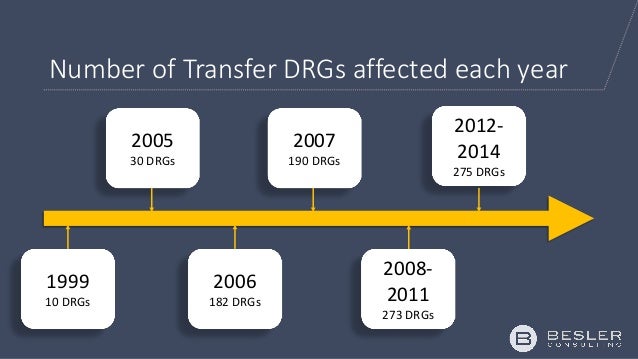
The DRG then the Transferring Hospital is paid based upon a per diem rate. 712008 Transfer DRGs originate from the Balanced Budget Act of 1997 and were created after Centers for Medicare. The patients principal diagnosis and up to 24 secondary diagnoses including any comorbidities or complications determine the DRG assignment.
In contrast for specified DRGs Medicare pays hospitals that transfer inpatients to certain post-acute care settings such as a skilled nursing facility or home health care a per diem rate for each day of the stay not to exceed the full DRG payment for a. Today I provide an overview of DRGs as well as AP-DRGs and APR-DRGs. 3M developed Diagnosis Related Groups DRGs to measures resource intensity of inpatient stays.